Relax...The Season Encourages It Epoch Times 2017 According to acupuncturist Ashley Flores, your fitness goals won’t be such a struggle when the yang seasons are on your side. She recommends starting an intense exercise regimen in the spring or summer, because more...

Homemade Chai Tea Recipe
I had my first taste of real, homemade chai while working at an Indian restaurant years and years ago. It was such a revelation after only having the boxed, overly sweetened, steamed milk concoction served by the big coffeehouse chains. This chai was...
Make Your Resolutions Work for Your Element
Use the 5 Element System to Help You Make More Productive Resolutions Confession time: I love New Year's resolutions. I find the process of imagining the coming year and writing lists of things I would like to accomplish very, well, fun. What can I say, finding the...

Yin and Yang in East Asian Medicine
The theory of Yin and Yang is one of the central philosophies in East Asian medicine, and a guide for diagnosis and treatment in acupuncture, herbal treatment, and Asian styles of massage. It is a way of looking at nature and the human body as pairs of opposite, but...
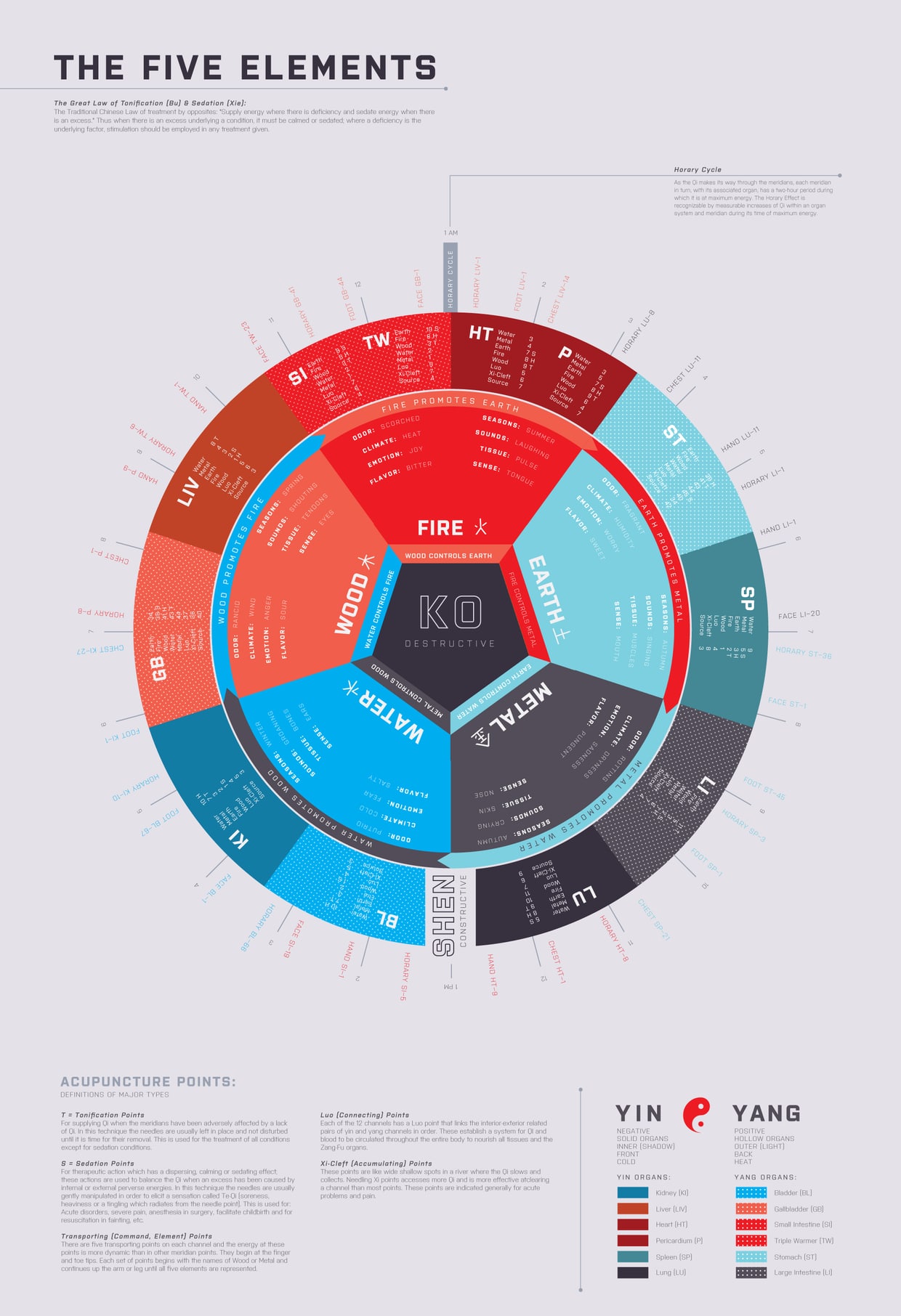
The 5 Elements at a Glance
Throughout the history of medicine, healers have classified qualities of health and disease according to 'elements'. Hippocratic medicine had the '4 humors' of earth, air, fire, and water that corresponded with the 4 seasons and qualities of emotion, colors, and type...

Acupuncture Lessens Side Effects of Chemotherapy
Cancer patients who receive chemotherapy treatment for their condition must withstand numerous side effects of the drugs, which interfere with work, daily and family life, and quality of life. Some side effects, including nausea and vomiting, and chemo-induced...
